A claims adjuster in Manchester recently told us something that perfectly captures the insurance industry’s biggest problem.
“I spent four hours yesterday processing a straightforward auto claim,” she said. “And you know what the crazy part is? Only 20 minutes of that was actually making decisions. The other three hours and forty minutes? Just finding information buried in documents.”
She’s not alone. Across insurance companies worldwide, highly trained professionals are spending 70-80% of their day hunting for data instead of using their expertise where it actually matters.
Meanwhile, Their competitors are processing those same 50 claims in under 4 hours total. Just Because they stopped manually processing documents and started using AI that actually understands insurance.
Here’s an uncomfortable fact: In an industry where claim settlement speed determines customer satisfaction, being 10x slower than your competitor isn’t a disadvantage … It’s an existential threat.
You’re about to see how automated document extraction is reshaping the way insurance claims are handled, the real tools insurers in Manchester and Hamilton are already using today, and why this approach can cut claim processing times almost immediately.
The Hidden Cost of “Just Doing Claims the Way We’ve Always Done Them”

Picture your typical Monday morning in a claims department:
Emma, your senior claims assessor, opens her inbox to find 43 new submissions. Each claim contains a chaotic mix of documents:
- Scanned police reports (some blurry, some sideways)
- Handwritten witness statements
- Medical certificates in 8 different formats
- Photos with crucial details buried in file names
- Policy documents requiring careful cross-referencing
- Third-party repair estimates on branded letterhead
Emma ends up having to open each document manually. Read through pages of text looking for key information. Type that information into your claims system. Cross-check policy coverage. Make notes. Route to the next person.
She can handle 8-12 claims per day if nothing goes wrong. (And usually things do go wrong)
Those 43 Monday morning claims? That’s a week of work. For one person. Just to get through Monday’s intake.
Meanwhile:
- Customers are calling asking “what’s the status?”
- Simple claims that should take hours are taking days
- Your team is working late just to stay current
- Complex claims requiring actual expertise get rushed because there’s no time
Sound familiar?
Here’s what most insurance executives don’t realize: this isn’t a staffing problem or a workflow problem. It’s a document problem.
What Document Intelligence Actually Means (Without the Tech Jargon)
Let’s clear something up right away: document intelligence isn’t another OCR tool that can barely read typed text, let alone someone’s scribbled notes on a claim form.
- Traditional OCR extracts text: “Claim Amount: $47,000.”
- Document intelligence understands context: this is a storm damage claim for $47,000 on a policy with $50,000 coverage and a $2,500 deductible, submitted by an approved contractor, with an incident date that falls within the policy period.
The difference matters. What took Emma 45 minutes of careful reading and system-hopping? Done in 8 seconds:
- Instant Classification The moment a document arrives, the system identifies what it’s looking at: FNOL form, medical report, repair estimate, police report, witness statement. It knows what information to expect and where to find it.
- Context-Aware Extraction It doesn’t just pull data, it interprets meaning. “Previous condition” in medical notes flags a potential pre-existing condition exclusion. “Passenger side damage noted” triggers a check against prior claims. The system understands insurance language and catches details that matter.
- Automatic Validation Extracted information gets cross-checked instantly: Does the claim amount exceed coverage limits? Is the incident date within the policy period? Is this the customer’s fifth similar claim? Are there coverage exclusions that apply?
- Intelligent Routing Based on what it finds, the system recommends action: auto-approve straightforward claims, flag suspicious patterns for review, route complex cases to specialists, highlight missing documentation.
Generic OCR might achieve 65% accuracy on insurance documents and still require extensive manual review. Purpose-built document intelligence delivers 95-98% accuracy and catches nuances that generic tools miss entirely.
This is the difference between automation that creates more work and automation that actually works.
Real Numbers That Makes CFOs Smile

We can’t share their name, but we can share their story.
A commercial brokerage in Auckland was processing 800 claims monthly with four assessors. High turnover. Mediocre satisfaction scores. Growing waiting list they couldn’t handle.
They implemented Kudra AI in September. Here’s what changed:
In just a couple months:
- Claims volume: 2,100 monthly (they started accepting new clients)
- Customer satisfaction: +42 NPS points
- Revenue: Up 32%
- Staff feedback: “I actually enjoy my job now. I focus on expertise, not data entry.”
The managing director told us: “We thought we’d need to hire 3-4 more people to grow. Instead, we invested in Kudra AI and became 3x more productive with our existing team. “
So How Does Document Intelligence Actually Works? (The Simple Explanation)
You don’t need to understand the technical details to benefit from document intelligence, but here’s a simple framework for how it transforms your claims process:
Stage 1: Smart Intake

What happens: Claims arrive via any channel (email, web form, mobile app, even fax). The AI instantly:
- Classifies every document (claim form, medical cert, photo, estimate, etc.)
- Extracts all relevant information (dates, amounts, names, policy numbers)
- Validates data quality (flags missing information or inconsistencies)
- Creates a complete digital claim file
What you see: A fully structured claim appears in your system, with all documents organized and key data already extracted. No manual data entry required.
Time saved: What took 20-30 minutes now takes 45 seconds.
Stage 2: Intelligent Analysis
What happens: The AI extracts the informations and analyzes the claim against:
- Policy terms and coverage limits
- Historical claim patterns
- Fraud indicators
- Regulatory requirements
- Your company’s specific business rules
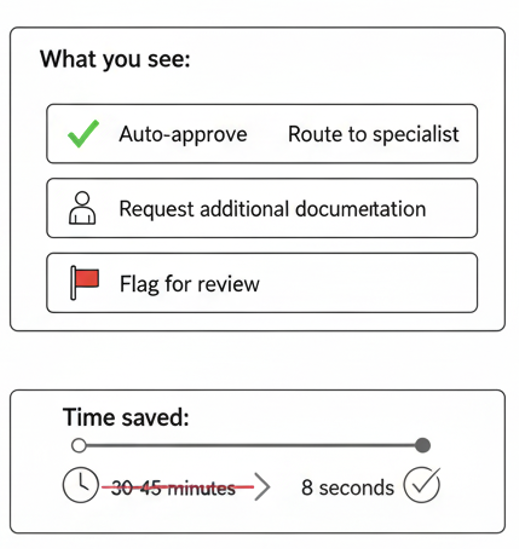
What you see: Clear recommendations: “Auto-approve,” “Route to specialist,” “Request additional documentation,” or “Flag for review.”
Time saved: What took 30-45 minutes of cross-referencing now takes 8 seconds.
Stage 3: Smart Routing
What happens: Based on the analysis, claims automatically flow to the right place:
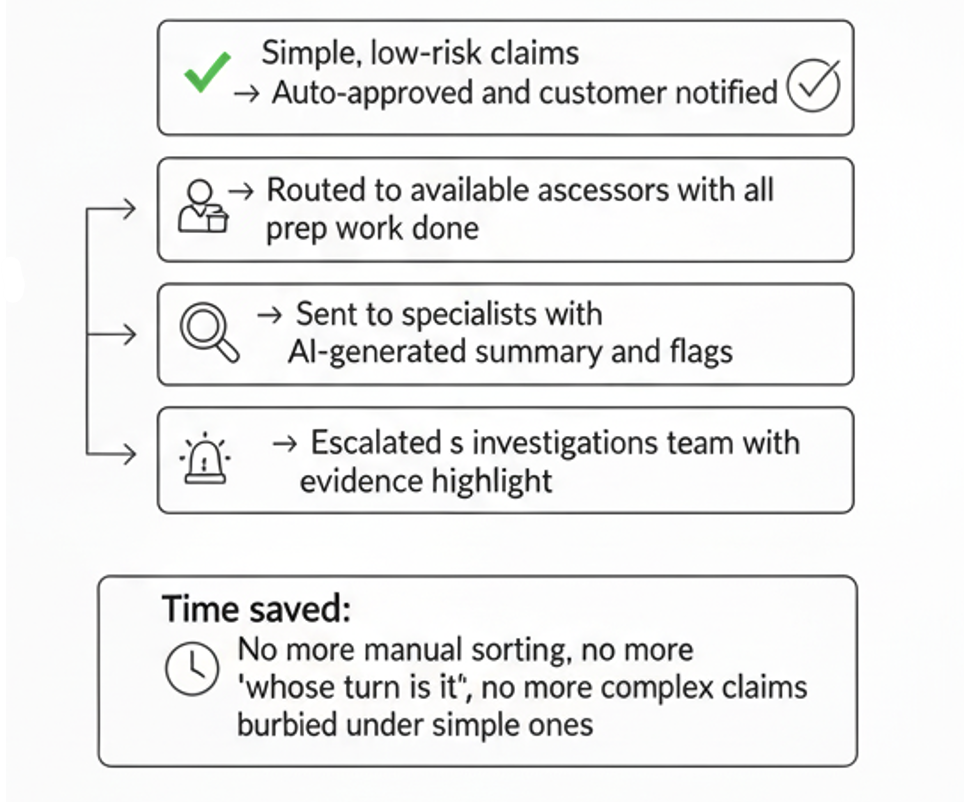
- Simple, low-risk claims → Auto-approved and customer notified
- Standard claims → Routed to available assessors with all prep work done
- Complex claims → Sent to specialists with AI-generated summary and flags
- Potential fraud → Escalated to investigations team with evidence highlighted
What you see: Your team’s queue is intelligently prioritized. Everyone works on claims that actually need human expertise.
Time saved: No more manual sorting, no more “whose turn is it,” no more complex claims buried under simple ones.
What Implementation Actually Looks Like
I know what you’re thinking: “This sounds amazing, but implementation will be a nightmare. Six months of consultants, system integration headaches, staff training, and everything breaking for the first three months.”
But the truth is it’s easier than you think … Here’s what actually happens with Kudra AI:
Week 1: Discovery & Setup
- We connect to your existing claims management system (via API or secure data transfer)
- You share sample documents (whatever you process regularly)
- We map your current workflow and identify automation opportunities
Your time investment: 3-4 hours of meetings. No technical expertise required.
Week 2-3: Custom Training
- We train AI models on your specific documents and terminology
- Fine-tune extraction accuracy for your most common claim types
- Set up Agentic AI validation based on your business requirements
- Configure routing logic to match your team structure
Your time investment: 2-3 hours of review and feedback. We handle all technical work.
Week 4: Rollout
- Lock in workflows that work best for your team
- We monitor system performance and suggest improvements
- Models automatically improve based on your team’s decisions
Your time investment: 30-minute quarterly check-ins. Everything else happens automatically.
Compare that to typical “enterprise AI” implementations that take 9-12 months, cost 3x as much, and still require a team of data scientists to maintain.
Your Next Step: See It In Action With Your Own Documents
I could write another 5,000 words about document intelligence, but here’s what actually matters: Does it work for your specific claims?
The best way to find out? Show us your most challenging documents and watch what happens.
Here’s what we’ll do:
Free Document Intelligence Assessment
- You send us 10-20 sample claims (anonymized, remove customer names/details)
- We process them through Kudra AI (takes about 15 minutes)
- We show you the results: extracted data, accuracy rates, processing time, automation potential
- We provide a custom ROI projection based on your actual documents and volumes
No sales pressure. No long-term commitment. Just a clear demonstration of what’s possible with your real-world claims.
The Future of Claims Processing Is Already Here
Five years from now, manual claims processing will seem as outdated as filing cabinets and fax machines. The insurance companies winning market share will all have one thing in common: they embraced document intelligence early, built competitive advantages, and never looked back.
The question isn’t whether your company will eventually use AI document intelligence. The question is: Will you be leading the transformation or scrambling to catch up?
The brokers and carriers implementing this technology right now aren’t just improving efficiency. They’re fundamentally reshaping their competitive position. Lower costs. Faster service. Happier customers. More growth with existing teams.
Meanwhile, manual processors are working harder, staying late, hiring constantly, and still falling behind.
Which future do you want?
Found This Helpful?
Book a free 30-minute discovery call to discuss how we can implement these solutions for your business. No sales pitch, just practical automation ideas tailored to your needs.
Book A Call