Introduction:
In the fast-paced world of insurance, efficiency and accuracy in claims processing can make or break a company's success. With the advent of advanced technologies, the insurance industry is undergoing a digital transformation, particularly in claims processing. Automation is key to streamlining this critical process, reducing costs, improving customer satisfaction, and enhancing overall operational efficiency. In this guide, we explore the latest trends and strategies for automating claims processing in 2024.
Claims Process Automation
Claims process automation involves using technology to automate manual tasks in the claims handling process. This can include everything from data collection and validation to claims assessment and settlement. By automating these tasks, insurers can reduce errors, save time, and enhance the overall customer experience.
Here is a straightforward explanation of how automation could simplify the claims process:
1. Data Collection and Intake:
Data collection and intake are crucial steps in the claims process, as they lay the foundation for the entire workflow. When a claim is submitted, OCR technology can extract key information, such as the claimant’s name, policy number, date of loss, and description of the incident, from scanned documents like police reports, medical records, and repair estimates. This eliminates the need for manual data entry, saving time and reducing the risk of errors.
2. Data Validation:
Data validation is critical to ensuring the accuracy and completeness of the collected data. Implement automated validation rules to check the accuracy and completeness of the collected data. These rules can verify data formats, validate ranges (such as dates or monetary values), and ensure that all required fields are filled out. If the automated validation rules detect any discrepancies or missing information, the system should flag these issues for manual review.
3. Claims Assessment:
Once the claim’s validity is established, the system can calculate the payout amount based on policy terms, coverage limits, and other relevant factors. Automation ensures accuracy and consistency in calculating payouts, reducing the risk of errors and ensuring fair settlements.
4. Decision Making:
After completing the assessment and validation stages, the insurer uses the gathered information to decide on the claim. This decision-making process can be automated, as the system applies predefined rules to determine the suitable payment amount or
level of coverage. For complex cases, route claims to human reviewers for manual assessment.
5. Settlement :
After approval of a claim, the automate tools can automatically start the payment process. Automation helps ensure that the correct amount is paid out based on the claim assessment and policy coverage. By linking the assessment results directly to the payment system, insurers can minimize errors and discrepancies in payouts.
6. Data-Driven Claims Analysis:
After processing, the automation software analyzes claims data to identify trends and patterns. This information helps improve claims processes, enhance fraud detection, and refine decision-making algorithms.
Benefits of Insurance Claims Processing Automation
Faster Claims Processing:
How Claims Processing Automation Accelerates the Customer Experience in Insurance Industry is by significantly reducing the time it takes to process a claim. Tasks that once required days or weeks can now be completed in a fraction of the time, leading to quicker claim resolutions and improved customer satisfaction.
∙ Improved Accuracy:
Automation reduces the risk of human error inherent in manual data entry and processing. By leveraging automated validation rules and algorithms, insurers can ensure that claims are processed accurately and in compliance with policy terms.
∙ Cost Savings:
Automation streamlines the claims process, reducing the need for manual intervention and the associated labor costs. Additionally, by preventing fraudulent claims and minimizing errors, insurers can save money on unnecessary payouts.
∙ Enhanced Customer Experience:
Automation leads to faster claim settlements and improved communication with customers. Policyholders can track the status of their claims in real-time, leading to greater transparency and trust in the insurance company.
∙ Improved Compliance:
Automation helps ensure that claims are processed in compliance with regulatory requirements and company policies plus that is how AI-Powered Fraud Detection in Insurance Claims works. By automatically applying the latest rules and regulations, insurers can avoid costly penalties and legal issues.
Automating the claims process has not only made it faster and more seamless but also liberated it from time constraints. Customers can now make claims 24/7, without having to wait for call center hours or agent availability.
Use Cases Examples
Policy administration and client servicing:
To maintain a competitive edge, insurance companies constantly strive to meet customer expectations. Leveraging software robots for swift and precise data analysis, insurers can proactively notify customers about potential losses before they occur. This proactive approach enhances customer satisfaction and loyalty.
Business and process analytics:
Efficient business processes are crucial for insurance companies to thrive. Automation tools offer the ability to track and record all activities, providing valuable insights for process improvement. By quantifying and appraising actions, these tools serve as reliable benchmarks for enhancing operational efficiency. Moreover, automated processes reduce the workload on employees, allowing them to focus more on delivering personalized services to clients.
Claims classification:
Claims management software plays a vital role in categorizing claims based on various criteria such as nature and severity. For example, claims in an insurance company can be classified as property damage, bodily injury, or medical claims. This classification streamlines claims processing and resource allocation, improving overall efficiency and customer satisfaction.
Claims Process Automation with Kudra
Kudra is a leading provider of claims process automation solutions, offering innovative tools to streamline and optimize the claims handling process. With Kudra’s advanced AI and machine learning capabilities, insurance companies can automate key aspects of claims processing, leading to faster claim resolution, reduced costs, and improved customer satisfaction. But How to Implement Claims Process Automation ?
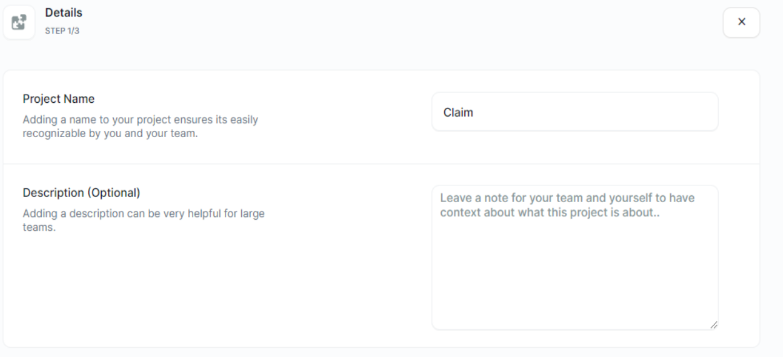
Create a new project
To get started, sign in to your Kudra.ai account or sign up if you’re new. When creating a new project, you’ll need to input information such as the project’s name, industry, and any specific parameters related to your document processing requirements.
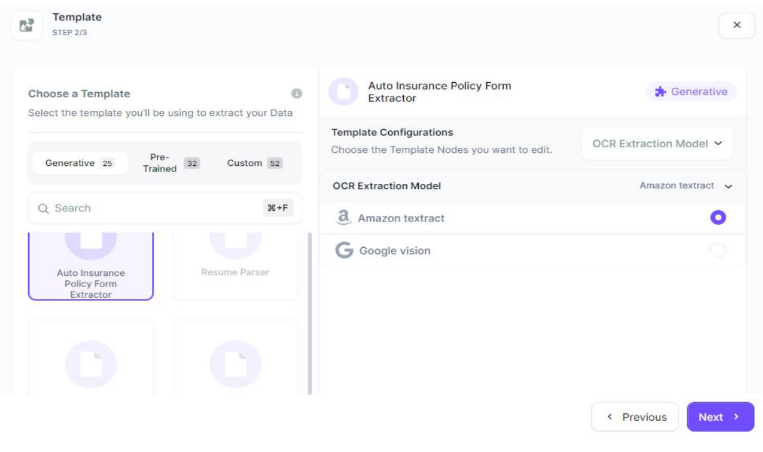
Choose your ideal template
Select your preferred template from Kudra.ai’s customizable options, specifically designed for various insurance document types. Customize the template to match the specific nuances and formatting requirements of your insurance documents
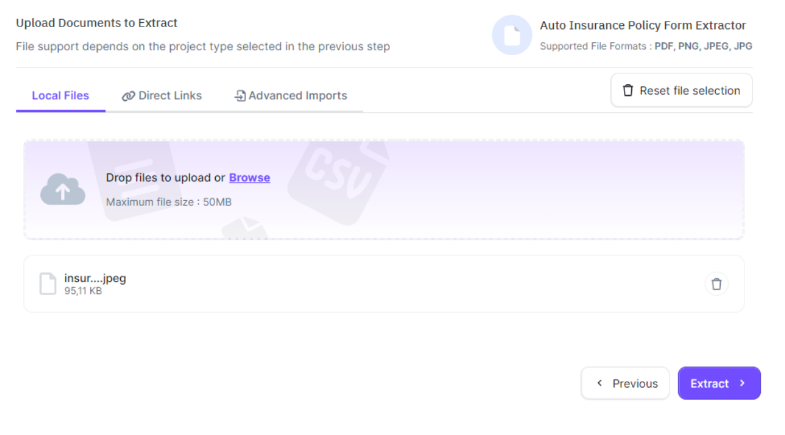
Upload your claims in a range of file formats, including PDFs or scanned images, using the user-friendly interface. Kudra.ai then automatically processes and extracts pertinent information from each document.
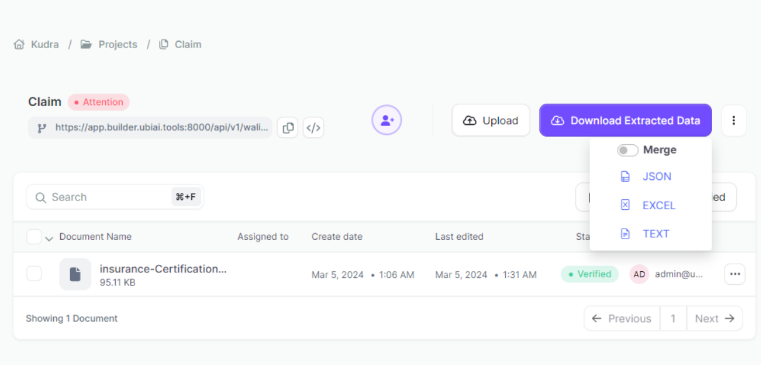
Effortlessly review the extracted data with Kudra.ai’s intuitive dashboard to ensure accuracy and completeness. With a simple click, you can verify that all information has been accurately extracted.
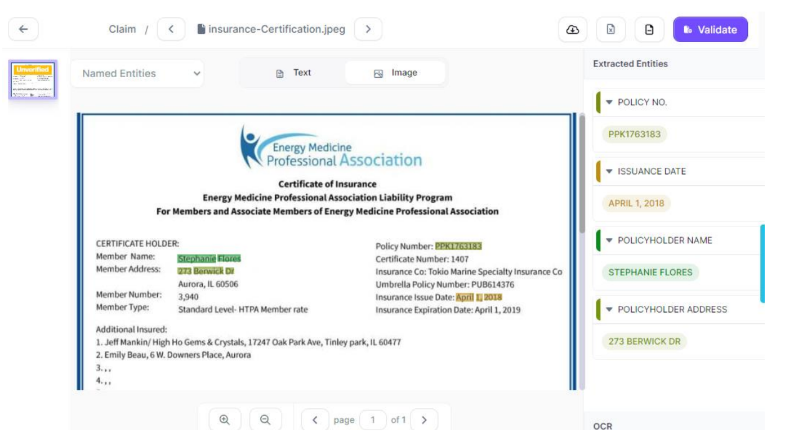
After the processing cycle is complete, access the organized and streamlined results. Kudra.ai presents the extracted data in a structured format, allowing for easy export, integration into your Document Management System, or further analysis as required.
Conclusion:
Claims process automation is no longer a luxury but a necessity for insurance companies looking to stay competitive in the digital age. By leveraging technologies such as AI, NLP, and ML, insurers can streamline their claims processing, reduce costs, and improve customer
satisfaction. Embracing automation is not just about adopting new technologies it’s about transforming the way insurance companies do business in the 21st century.
